Bladder Control Problems: Causes, Medical Options, and How People Decide What to Do Next.
Bladder control problems (urinary incontinence) are more common than most people realize, yet they are rarely talked about openly. Many people live with symptoms for years before asking questions, often assuming that leakage, urgency, or frequent bathroom trips are just part of aging or something they have to tolerate.
Bladder control issues can affect daily routines, sleep, work, travel, social events, and confidence. They can also signal underlying health issues that deserve attention. Understanding what is happening, why it happens, and what types of medical approaches exist is often the first step toward making informed choices.
This page is designed to explain bladder control problems in clear language, outline common medical evaluation and treatment approaches, and help readers understand how decisions are typically made in clinical settings.
This information is educational only and is not medical advice. Diagnosis and treatment decisions must be made with a qualified medical professional.
What Are Bladder Control Problems?

Bladder control problems, also called urinary incontinence, refer to difficulty holding urine until an appropriate time and place. This can include leaking urine, feeling sudden urges that are hard to control, or needing to urinate much more often than normal.
From a medical perspective, bladder control relies on coordination between muscles, nerves, and the brain. When that coordination is disrupted, symptoms can occur.
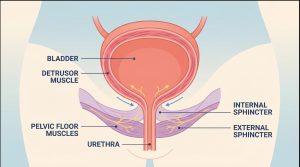
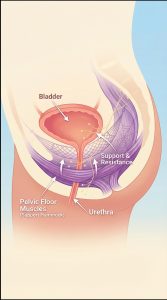
In everyday terms, the bladder is like a storage tank, the pelvic floor muscles act like a support hammock, and the nervous system acts like a signal system that tells everything when to tighten or relax. If any part of that system is not working as intended, control can be affected.
What Are Common Types of Bladder Control Problems?
Doctors often group bladder control issues into categories to help guide evaluation and treatment.
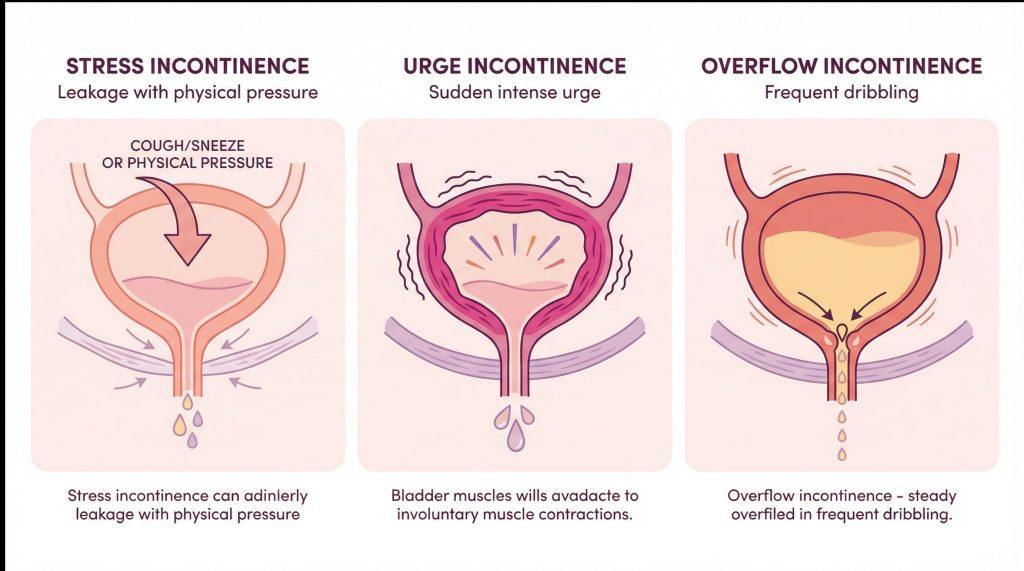
Stress incontinence
Leakage that occurs with physical pressure such as coughing, laughing, sneezing, or lifting.
Plain language explanation:
The muscles and tissues that support the bladder are not providing enough resistance during pressure.
Urge incontinence
A sudden, intense urge to urinate followed by leakage.
Plain language explanation:
The bladder muscle contracts when it should not, even if the bladder is not full.
Overflow incontinence
Frequent dribbling or inability to fully empty the bladder.
Plain language explanation:
The bladder fills beyond capacity because it does not empty properly.
Mixed incontinence
A combination of more than one type.
Understanding the type of symptoms someone has helps guide what tests or evaluations might be appropriate.
Why Are Bladder Control Problems Often Delayed or Ignored?
Many people delay seeking care because symptoms develop gradually. Others feel embarrassment or assume the issue is not serious enough to discuss.
Common reasons people wait include:
- Belief that symptoms are a normal part of aging
- Fear of surgery or medications
- Not knowing which type of doctor to see
- Assuming nothing can be done
Medical research from institutions such as the Cleveland Clinic and Johns Hopkins shows that early evaluation often opens more conservative and lower risk management options.
How Bladder Problems Are Evaluated in Medical Settings
Doctors do not guess when evaluating bladder symptoms. They gather information systematically.
Common evaluation steps may include:
- Medical history and symptom patterns
- Physical examination
- Urine testing to rule out infection
- Bladder diaries that track timing and volume
- Specialized testing such as urodynamic studies
Urodynamic testing is a medical term for measuring how the bladder fills and empties.
Plain language explanation:
These tests check how well the bladder stores urine and how effectively it releases it.
Not everyone needs advanced testing. The decision depends on symptoms, severity, and overall health.
General Categories of Treatment Approaches
Bladder control treatment is not one size fits all. Doctors typically begin with the least invasive options and escalate only if needed.
General categories include:
Behavioral and Lifestyle Approaches
These may focus on fluid timing, bladder training, and muscle coordination strategies.
Plain language explanation:
Small changes in habits and routines can reduce symptoms for some people.
Physical therapy focused on pelvic floor function
Specialized therapists work on muscle strength, coordination, and relaxation.
Plain language explanation:
This is not general exercise. It targets muscles most people do not realize they have.
Medical management
Doctors may discuss medications or other therapies depending on diagnosis.
Advanced interventions
For certain cases, procedures or implantable therapies may be considered after thorough evaluation.
This site does not recommend specific treatments. Decisions must be made with a qualified healthcare provider.
How People Typically Decide What Path to Take
Medical decisions often involve balancing:
- Severity of symptoms
- Impact on daily life
- Risk tolerance
- Reversibility of treatment
- Long term goals
Some people prioritize conservative options. Others seek faster symptom control. There is no universal right answer, only informed choices.
That is why understanding the full range of options matters.
When Bladder Symptoms May Signal Something More

While many bladder issues are not dangerous, certain symptoms should prompt timely medical evaluation.
These include:
- Blood in urine
- Pain with urination
- Sudden changes in bladder habits
- Neurological symptoms such as numbness or weakness
These symptoms do not automatically mean something serious, but they warrant professional evaluation.